24 maart 2019: lees ook dit artikel:
30 september 2017: Lees ook dit artikel:
Verder is deze overzichtsstudie: Targeted therapy of ovarian cancer including immune check point inhibitor wellicht interessant eens te bekijken:.
In dit studierapport worden gerichte behandelingen (tageted therapies) zoals Avastin - Bevacizumab, Pazopanib, Cediranib en Parpremmers zoals olaparib en rucaparib of combinaties van beide soorten medicijnen al of niet in combinatie met chemo besproken aan de hand van de literatuur - studies die tot nu toe daarmee zijn gedaan.
Ook immuuntherapie met anti-PD-medicijnen wordt in dit studierapport besproken. Zie onderaan dit artikel abstract en referentielijst van dit studierapport.
4 maart 2016: Bron: JCO December 1, 2015 vol. 33 no. 34 4015-4022
Immuuntherapie met nivolumab, een anti-PD medicijn, geeft ook bij zwaar voorbehandelde, platinum resistente eierstokkankerpatiënten uitstekende en hoopvolle resultaten. Uit een grotere fase III studie van nivolumab bij solide tumoren zijn 20 patienten met eierstokkanker opgenomen in een fase II studie en in een evalutatie na drie jaar blijken alsnog 2 patiënten een duurzame complete remissie te hebben bereikt. En 45% van de 20 patienten kregen met nivolumab controle over de ziekte, dus er was geen progressie van de ziekte. De mediane progressie-vrije ziekte was 3.5 maanden (95% CI, 1.7 tot 3.9 maanden), en de mediane overall overleving was 20.0 maanden (95% CI, 7.0 maanden tot nog niet bereikt) op moment van de studie analyse.
Bedenk hierbij dat deze studie is uitgevoerd bij patiënten die al een hele rits aan chemobehandelingen hebben gehad en in het laatste stadium van hun ziekte verkeerden. Dat dan alsnog 2 patienten een complete remissie bereikten, dus geen aantoonbare kanker meer en die nog steeds voortduurt al meer dan 20 maanden, is bijna een wonder te noemen. 2 uit 20 patienten is 10% en een aantal patiënten bewerkstelligde ook een gedeeltelijke remissie (50% of meer tumorvermindering). Overall bereikte 15% een duurzame gedeeltelijke of complete remissie, schrijven de onderzoekers. 45 % kreeg met nivolumab controle over de ziekte.
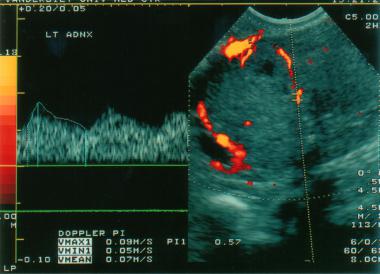
Foto: Transvaginal, color Doppler ultrasonogram shows a solid mass in the left ovary. Low impedance flow is noted within this mass, which is a clear cell carcinoma of the ovary.
Er was vantevoren niet gecheckt op de PD-L1 mutatie of althans niet kort voordat de nivolumab behandeling startte. Er is inmiddels een fase III studie opgezet waarin grotere aantallen patienten met eierstokkanker worden opgenomen en waarbij voor de start van de behandeling aan de hand van recent tumorweefsel de PD-L1 mutatie zal worden gecheckt.
Voor onze donateurs hebben wij het volledige studierapport: Safety and Antitumor Activity of Anti–PD-1 Antibody, Nivolumab, in Patients With Platinum-Resistant Ovarian Cancer opgevraagd en gekregen.
Mocht u dit studierapport willen hebben stuur me dan maar een mailtje: redactie@kanker-actueel.nl
Het abstract van de studie staat hieronder.
The encouraging safety and clinical efficacy of nivolumab in patients with platinum-resistant ovarian cancer indicate the merit of additional large-scale investigations
- © 2015 by American Society of Clinical Oncology
Safety and Antitumor Activity of Anti–PD-1 Antibody, Nivolumab, in Patients With Platinum-Resistant Ovarian Cancer
- Junzo Hamanishi⇑,
- Masaki Mandai,
- Takafumi Ikeda,
- Manabu Minami,
- Atsushi Kawaguchi,
- Toshinori Murayama,
- Masashi Kanai,
- Yukiko Mori,
- Shigemi Matsumoto,
- Shunsuke Chikuma,
- Noriomi Matsumura,
- Kaoru Abiko,
- Tsukasa Baba,
- Ken Yamaguchi,
- Akihiko Ueda,
- Yuko Hosoe,
- Satoshi Morita,
- Masayuki Yokode,
- Akira Shimizu,
- Tasuku Honjo and
- Ikuo Konishi
+ Author Affiliations
- Corresponding author: Junzo Hamanishi, MD, PhD, Department of Gynecology and Obstetrics, Kyoto University Graduate School of Medicine, 54 Kawahara-cho, Shogoin, Sakyo-ku, Kyoto, Kyoto 606-8507, Japan; e-mail: jnkhmns@kuhp.kyoto-u.ac.jp.
-
Both J.H. and M.M. contributed nearly equally to this work.
Abstract
Purpose Programmed death-1 (PD-1), a coinhibitory immune signal receptor expressed in T cells, binds to PD-1 ligand and regulates antitumor immunity. Nivolumab is an anti–PD-1 antibody that blocks PD-1 signaling. We assessed the safety and antitumor activity of nivolumab in patients with platinum-resistant ovarian cancer.
Patients and Methods Twenty patients with platinum-resistant ovarian cancer were treated with an intravenous infusion of nivolumab every 2 weeks at a dose of 1 or 3 mg/kg (constituting two 10-patient cohorts) from October 21, 2011. This phase II trial defined the primary end point as the best overall response. Patients received up to six cycles (four doses per cycle) of nivolumab treatment or received doses until disease progression occurred. Twenty nivolumab-treated patients were evaluated at the end of the trial on December 7, 2014.
Results Grade 3 or 4 treatment-related adverse events occurred in eight (40%) of 20 patients. Two patients had severe adverse events. In the 20 patients in whom responses could be evaluated, the best overall response was 15%, which included two patients who had a durable complete response (in the 3-mg/kg cohort). The disease control rate in all 20 patients was 45%. The median progression-free survival time was 3.5 months (95% CI, 1.7 to 3.9 months), and the median overall survival time was 20.0 months (95% CI, 7.0 months to not reached) at study termination.
Conclusion This study, to our knowledge, is the first to explore the effects of nivolumab against ovarian cancer. The encouraging safety and clinical efficacy of nivolumab in patients with platinum-resistant ovarian cancer indicate the merit of additional large-scale investigations (UMIN Clinical Trials Registry UMIN000005714).
Footnotes
-
See accompanying editorial on page 3987
-
Supported by research funds from Health and Labour Sciences Research Grant No. 11104959 (to J.H. and I.K.); by Translational Research Network Program of the Ministry of Education, Culture, Sports, Science and Technology of Japan Grant No. 2013037 (to J.H. and I.K.); and by Kyoto University grants.
-
Terms in blue are defined in the glossary, found at the end of this article and online at www.jco.org.
-
Authors' disclosures of potential conflicts of interest are found in the article online at www.jco.org. Author contributions are found at the end of this article.
-
Glossary Terms
- CA-125 (cancer antigen 125):
- a protein produced by the fallopian tubes, the endometrium, and the lining of the abdominal cavity (peritoneum). CA-125 is a tumor marker present in higher than normal amounts in the blood and urine of patients with certain cancers. Typically, women with ovarian cancer have high levels of CA-125. Other conditions associated with elevated levels of CA-125 include endometriosis, pancreatitis, pregnancy, normal menstruation, and pelvic inflammatory disease. CA-125 levels may be used to help diagnose ovarian cancer and to determine whether these tumors are responding to therapy. The normal range for CA-125 is less than 35 U/mL and less than 20 U/mL for women who have been treated for ovarian cancer. Women with ovarian cancer may show values higher than 65 U/mL.
- CD8+ T cell:
- cytotoxic T cell that is the primary effector cells of the immune system. They are characterized by the presence of the CD8 cell-surface marker.
- Computed tomography (CT) scan:
- a series of pictures created by a computer linked to an x-ray machine taken of the inside of the body from different angles.
- FIGO staging:
- a tumor staging system established and revised by the International Federation of Gynecology and Obstetrics (FIGO) that takes into account the postoperative histopathologic evaluation of the specimen. The FIGO stage classification has prognostic value.
- Immune checkpoint:
- immune inhibitory pathway that negatively modulates the duration and amplitude of immune responses. Examples include the CTLA-4:B7.1/B7.2 pathway and the PD-1:PD-L1/PD-L2 pathway.
- Immunohistochemistry:
- the application of antigen-antibody interactions to histochemical techniques. Typically, a tissue section is mounted on a slide and incubated with antibodies (polyclonal or monoclonal) specific to the antigen (primary reaction). The antigen-antibody signal is then amplified using a second antibody conjugated to a complex of peroxidase-antiperoxidase, avidin-biotin-peroxidase, or avidin-biotin alkaline phosphatase. In the presence of substrate and chromogen, the enzyme forms a colored deposit at the sites of antibody-antigen binding. Immunofluorescence is an alternate approach to visualize antigens. In this technique, the primary antigen-antibody signal is amplified using a second antibody conjugated to a fluorochrome. On ultraviolet light absorption, the fluorochrome emits its own light at a longer wavelength (fluorescence), thus allowing localization of antibody-antigen complexes.
- Immunotherapy:
- a therapeutic approach that uses cellular and/or humoral elements of the immune system to fight a disease.
- PD-1:
- programmed cell death protein 1 (CD279), a receptor expressed on the surface of activated T, B, and NK cells that negatively regulates immune responses, including autoimmune and antitumor responses.
- PD-L1:
- programmed cell death 1 ligand 1 (CD274; also known as B7-H1), the major binding partner (ligand) for the PD-1 inhibitory immune receptor. PD-L1 is expressed on the surface of activated antigen presenting cells, such as dendritic cells, and by many types of cancer cells. Its expression is induced by the inflammatory cytokine interferon-alfa
- RECIST (Response Evaluation Criteria in Solid Tumors):
- a model proposed by the Response Evaluation Criteria Group by which a combined assessment of all existing lesions, characterized by target lesions (to be measured) and nontarget lesions, is used to extrapolate an overall response to treatment.
As demonstrated in recent clinical trials, the use of bevacizumab, cediranib, pazopanib, olaparib, and rucaparib, either alone or in combination with conventional cytotoxic agents, improves progression-free survival. Trials on immune checkpoint inhibitors such as nivolumab have revealed prolonged responses in a small set of ovarian cancer cases but require further exploration. In this review, we discuss the role of targeted therapies against ovarian cancer, including the use of immune checkpoint inhibitors.
Targeted therapy of ovarian cancer including immune check point inhibitor
Abstract
Epithelial ovarian cancer is the eighth most common cause of cancer-related deaths in women because most patients present with advanced stage disease at the time of diagnosis. Although cytoreductive surgery and platinum-based chemotherapy remain the gold standards of treatment, the recurrence rate of ovarian cancer remains high. Attempts to improve this standard two-drug chemotherapy by adding a third cytotoxic drug have failed to affect either progression-free survival or overall survival and have resulted in an increase in toxic side effects. Some anti-angiogenic agents, poly(ADP-ribose) polymerase, and immune checkpoint inhibitors have shown efficacy in early stages of development for the treatment of epithelial ovarian cancer. As demonstrated in recent clinical trials, the use of bevacizumab, cediranib, pazopanib, olaparib, and rucaparib, either alone or in combination with conventional cytotoxic agents, improves progression-free survival. Trials on immune checkpoint inhibitors such as nivolumab have revealed prolonged responses in a small set of ovarian cancer cases but require further exploration. In this review, we discuss the role of targeted therapies against ovarian cancer, including the use of immune checkpoint inhibitors.
REFERENCES
Gerelateerde artikelen
- Onderzoekers ontdekken waarom immuuntherapie bij eierstokkanker soms wel en soms niet werkt. Aangeboren immuniteit speelt grotere rol dan verworven immuniteit bij eierstokkanker en immuuntherapie.
- Overzichtstudie van vormen van immuuntherapie bij eierstokkanker in alle stadia, waaronder dendritische celtherapie, CAR-T celtherapie en immuuntherapie met anti-PD medicijnen.
- Pembrolizumab, een anti-PD medicijn bij zwaarvoorbehandelde eierstokkankerpatienten geeft toch nog bij een derde van de patienten stabiele ziekte en een betere mediane overall overleving
- Dendritische celtherapie aanvullend op chemo verbetert overall overleving op 2-jaar met 32 procent (73 vs 41 procent) bij gevorderde eierstokkanker.
- Immuuntherapie met avelumab, een anti-PD medicijn blijkt veilig en geeft hoopvolle resultaten bij patienten met zwaar voorbehandelde vergevorderde eierstokkanker
- Nivolumab, immuuntherapie met anti-PD medicijn geeft hoopvolle resultaten bij zwaar voorbehandelde platinum resistente eierstokkankerpatienten
- DMUC5754A een nieuw experimenteel medicijn blijkt effectief bij eierstokkanker met een stadium van resistentie van op platinum gebaseerde chemo - taxol
- Dendritische celtherapie blijkt succesvolle aanpak voor eierstokkanker bewijst fase II studie
- Immuuntherapie met p53-SLP-vaccin zou volgens promovenda Renee Vermeij veelbelovende behandeling zijn, maar eerdere fase II studie laat zien dat er geen therapeutisch effect is met deze aanpak
- Immuuntherapie: Antibody therapie kan het positieve effect van een vaccin vergroten blijkt uit studies met uitbehandelde eierstokkankerpatienten (graad IV) en melanoompatienten. Veel patienten hebben er veel baat bij zonder bijwerkingen.
- Studie suggereert dat eierstokkankercellen zich via een eigen te produceren eiwit - collageen IV - dusdanig kunnen aanpassen dat immuniteit voor chemo ontstaat.
- Ovarex - oregovomab een immuunstimulerend middel - stimulatie T-cellen - geeft niet significant langere overleving bij gevorderde eierstokkanker aldus fase II studie, maar wel verdubbeling van ziektevrije tijd
- Ovarex - oregovomab, een immuunstimulerend middel - stimulatie T-cellen - geeft significant langere overleving bij gevorderde eierstokkanker aldus fase II studie. Vervolgstudies kunnen dit goede effect neit bevestigen.
- Interferon-alpha (INF) na operatie en - of chemo bij eierstokkanker is zinloos en geeft geen enkele meerwaarde aan behandeling van eierstokkanker, aldus fase III studie van 7 jaar.
- Immuuntherapie of gerichte - targeted therapie bij eierstokkanker: een overzicht van belangrijke studies en recente ontwikkelingen, ook in het kader van personalised medicine



Plaats een reactie ...
Reageer op "Nivolumab, immuuntherapie met anti-PD medicijn geeft hoopvolle resultaten bij zwaar voorbehandelde platinum resistente eierstokkankerpatienten"