18 februari 2015: bron: European Prospective Investigation Into Cancer and Nutrition (EPIC)
Wanneer vrouwen veel foliumzuur nemen via voeding dan verminderen zij significant het risico op hormoonreceptor negatieve borstkanker te krijgen voor zij in de overgang komen. Dit blijkt uit een langjarige - 11,5 jaar - studie in tien verschillende Europese landen onder totaal 367,993 vrouwen.
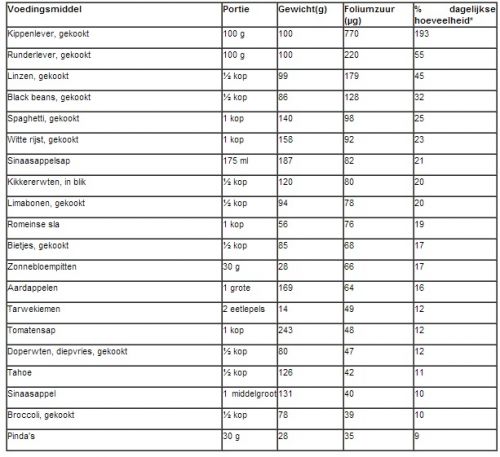
Foliumzuur komt voor in bepaalde groenten en fruit maar ook veel in gekookte kippenlever en gekookte runderlever. Zie hier een tabel van de website over foliumzuurbijkinderwens:
Studieresultaten:
Vrouwen in het hoogste quintile van foliumzuurinname hadden net een significant verminderd risico op borstkanker overall versus vrouwen in het laagste quintile (hazard ratio = 0.92, 95% confidence interval = 0.83–1.01, P = .037 for trend).
Premenopausale vrouwen (vrouwen voor de overgang) in het hoogste versus laagste quintile hadden een significant verminderd risico op het ontwikkelen van hormoon-receptorn-negatieve borstkanker (AR neg.) (HR = 0.66, 95% CI = 0.45–0.96, P = .042 for trend) en progesteron receptor–negatieve borstkanker (PR-neg) (HR = 0.70, 95% CI = 0.51–0.97, P = .021 for trend).
er werd geen significant verschil gevonden op het risico op borstkanker bij vrouwen na de overgang.
Onder vruwen die veel alcohol gebruikten (meer dan 12 alcoholische drankjes per week), hadden die vrouwen in het hoogste quintile van inname van folliumzuur versus laagste quintile een significant verminderd risico op borstkanker overall. (HR = 0.86, 95% CI = 0.75–0.98, P = .035 for interaction).
Conclusie:
De onderzoekers concluderen dan ook : “Hoge inname van foliumzuur via voeding is gerelateerd aan een verminderd risico op receptor-negatieve borstkanker bij premenopauzale vrouuwen .”
Het volledige studierapport: Dietary Folate Intake and Breast Cancer Risk: European Prospective Investigation Into Cancer and Nutrition is tegen betaling in te zien.
Hier het abstract van deze studie:
“Higher dietary folate intake may be associated with a lower risk of sex hormone receptor–negative breast cancer in premenopausal women.”
Source:
-
JNCI J Natl Cancer Inst (2015) 107 (1): dju367 doi: 10.1093/jnci/dju367
Dietary Folate Intake and Breast Cancer Risk: European Prospective Investigation Into Cancer and Nutrition
- J. de Batlle,
- P. Ferrari,
- V. Chajes,
- J. Y. Park,
- N. Slimani,
- F. McKenzie,
- K. Overvad,
- N. Roswall,
- A. Tjønneland,
- M. C. Boutron-Ruault,
- F. Clavel-Chapelon,
- G. Fagherazzi,
- V. Katzke,
- R. Kaaks,
- M. M. Bergmann,
- A. Trichopoulou,
- P. Lagiou,
- D. Trichopoulos,
- D. Palli,
- S. Sieri,
- S. Panico,
- R. Tumino,
- P. Vineis,
- H. B. Bueno-de-Mesquita,
- P. H. Peeters,
- A. Hjartåker,
- D. Engeset,
- E. Weiderpass,
- S. Sánchez,
- N. Travier,
- M. J. Sánchez,
- P. Amiano,
- M. D. Chirlaque,
- A. Barricarte Gurrea,
- K. T. Khaw,
- T. J. Key,
- K. E. Bradbury,
- U. Ericson,
- E. Sonestedt,
- B. Van Guelpen,
- J. Schneede,
- E. Riboli and
- I. Romieu
+ Author Affiliations
- Correspondence to: Jordi de Batlle, PhD, International Agency for Research on Cancer, 150 cours Albert Thomas, Lyon 69008, France (e-mail: jordidebatlle@gmail.com).
- Received January 16, 2014.
- Revision received May 30, 2014.
- Accepted October 6, 2014.
Abstract
Background: There is limited evidence on the association between dietary folate intake and the risk of breast cancer (BC) by hormone receptor expression in the tumors. We investigated the relationship between dietary folate and BC risk using data from the European Prospective Investigation into Cancer and Nutrition (EPIC).
Methods: A total of 367993 women age 35 to 70 years were recruited in 10 European countries. During a median follow-up of 11.5 years, 11575 women with BC were identified. Dietary folate intake was estimated from country-specific dietary questionnaires. Cox proportional hazards regression models were used to quantify the association between dietary variables and BC risk. BC tumors were classified by receptor status. Subgroup analyses were performed by menopausal status and alcohol intake. Intake of other B vitamins was considered. All statistical tests were two-sided.
Results: A borderline inverse association was observed between dietary folate and BC risk (hazard ratio comparing top vs bottom quintile [HRQ5-Q1] = 0.92, 95% CI = 0.83 to 1.01, P trend = .037). In premenopausal women, we observed a statistically significant trend towards lower risk in estrogen receptor-negative BC (HRQ5-Q1 = 0.66, 95% CI = 0.45 to 0.96, P trend = .042) and progesterone receptor-negative BC (HRQ5-Q1 = 0.70, 95% CI = 0.51 to 0.97, P trend = .021). No associations were found in postmenopausal women. A 14% reduction in BC risk was observed when comparing the highest with the lowest dietary folate tertiles in women having a high (>12 alcoholic drinks/week) alcohol intake (HRT3-T1 = 0.86, 95% CI = 0.75 to 0.98, P interaction = .035).
Conclusions: Higher dietary folate intake may be associated with a lower risk of sex hormone receptor–negative BC in premenopausal women.
- © The Author 2014. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
Gerelateerde artikelen
- Alcohol tast de darmbiotica aan en geeft hoger risico op ziektes. Blijkt uit verschillende studies.
- ALDH4A1, een veel voorkomend enzym - eiwit speelt een verrassende rol in het voorkomen van kanker.
- Algemeen: Iedereen van jong tot oud kan het functioneren en de gezondheid van de hersenen op eenvoudige manier verbeteren ongeacht de leeftijd
- Algemeen: Aangepast voedingspatroon en meer beweging onder telefonische en schriftelijke begeleiding verbetert significant kwaliteit van leven en functioneren van oudere overlevenden van borstkanker en prostaatkanker met overgewicht en slechte levensstijl
- Algemeen: Wat is er met ons voedsel gebeurd? Een desastreuze ontwikkeling lijkt. ODE publiceerde in 2004 een artikel over afname van voedingstoffen van groenten en fruit dat nog steeds actueel lijkt.
- Bloedverdunners die vitamine K in het lichaam remmen worden gelinkt aan een verhoogd risico voor het ontwikkelen en verergeren van (osteo)artrose.
- Boter vervangen door plantaardige olie om te bakken en frituren geeft 17 procent lager risico op sterven aan kanker en overlijden in het algemeen
- Caffeine: mensen met een dieet met een hoog cafeïnegebruik, hebben een rijkere darmflora, met hogere waarden van mogelijk ontstekingsremmende bacteriën, vergeleken met dieet met weinig cafeïne.
- Darmflora: Alzheimerpatiënten missen goede bacterie in hun darmen, die gezonde mensen wel hebben. Veel vezels en gevarieerd eten zou Alzheimer kunnen voorkomen
- Darmflora beinvloed door voeding en leefstijl speelt cruciale rol in ontstaan van ziektes ook bij ontstaan van kanker en behandelingen daarvan
- Deze 6 wetenschappelijke onderzoeken over fysiologisch actieve (voedings)stoffen, zoals vitamines en andere supplementen en toepassingen ervan in de praktijk zijn genomineerd voor de James Lindprijs 2021.
- Dierlijke vetten, roken en leefstijl zijn de belangrijkste factoren die bepalen of iemand kanker krijgt of niet. Blijkt uit heel groot wereldwijd uitgevoerd onderzoek in 187 landen
- Een nieuw drinkvoedingsproduct, met wei-eiwitten, vrije vertakte aminozuren en ursolzuur, verbetert de loopsnelheid en mitochondrieel functioneren van ondervoede ouderen in vergelijking met een standaard drinkvoedingsproduct.
- Eenzaamheid en te weinig sociale contacten blijken grootste risico op overlijden aan alle oorzaken bij mensen met zwaarlijvigheid en obesitas
- Foliumzuur via voeding geeft significant minder risico op hormoon-receptor-negatieve borstkanker bij vrouwen in leeftijd voor de overgang
- Foliumzuur - vitamine B speelt cruciale rol bij optredende mutaties in genen die gerelateerd zijn aan risico op kanker en specifiek bij borstkanker.
- Groene thee vermindert kans op vormen van spijsverteringskanker met gemiddeld 20 procent bij oudere Chinese vrouwen copy 1
- Insulineresistentie: meer dan diabetes type 2. Schatting is dat zeg 75 procent van de Nederlandse bevolking een vorm van insulineresistentie heeft.
- koffieconsumptie lijkt een beschermende factor te zijn tegen de ziekte van Alzheimer en achteruitgang in cognitieve functies.
- Koffie zou het risico op ontstaan van buikvlieskanker met 18 procent kunnen verminderen bewijst een deelstudie uit de Nurses Health Study
- Maak dringend meer werk van gezondheid als onderdeel van bestaanszekerheid, schrijft de Sociaal Economische Raad (SER) in nieuw beleidsrapport
- Mediterraan dieet voorkomt bij vrouwen die dit gebruiken vanaf middelbare leeftijd chronische ziektes en geeft veel betere gezondheid op 70 jaar en ouder
- Mediteraan voedingspatroon kan sterfte aan kanker met 35 procent verminderen in vergelijking met westers dieet.
- Mineralen: De belangrijkste mineralen die de westerse mens dagelijks nodig heeft op een rijtje gezet.
- Multivitamine met mineralen (MVM) gedurende 3 jaar dagelijks ingenomen verminderde bij ouderen (65+) met 60 procent mentale achteruitgang in vergelijking met placebo
- Nitisinon - Orfadin een geneesmiddel tegen een stofwisselingsziekte blijkt in bloed dodelijk voor muggen die malaria verspreiden
- Onderzoek naar effect van voeding op kanker verhelderend. prof. dr. J.W. Coebergh voorspelt de trends van kanker incidentie en kanker bij ouderen. Wat werkt wel en wat werkt niet.
- Overgewicht komt vaker voor dan ondergewicht wereldwijd blijkt uit groot wereldwijd uitgevoerd onderzoek
- RIVM heeft een nieuwe versie van Nederlands Voedingsstoffenbestand (NEVO) gepubliceerd. Hierin informatie over 2152 voedingsmiddelen, waarvan 181 nieuwe producten.
- Plantaardig dieet en tomaten verminderen kans op krijgen van prostaatkanker
- Rapport de Lancet Countdown van VN-klimaatpanel IPCC stelt dat miljoenen doden worden veroorzaakt door slechte luchtkwaliteit, hittegolven en andere gevolgen van CO2-uitstoot waarvan vele doden hadden voorkomen kunnen worden
- Rood vlees en bewerkt vlees verhoogt kans op blaaskanker met 25 tot 33 procent
- Regelmatig noten eten verlaagt de kans om te overlijden aan een hart- of vaatziekte met 29 procent of aan kanker met 11% in vergelijking met mensen die weinig tot geen noten eten
- Screening en diagnostiek via bevolkingsonderzoeken en scans loopt de spuigaten uit en maakt iedere nederlander bijna ziek, stelt de Raad voor Volksgezondheid en Samenleving in een rapport
- Sterk bewerkte voeding en voedingsproducten veroorzaken meer sterfgevallen aan kanker, vooral bij vrouwen met eierstokkanker was de sterfte hoger blijkt uit bevolkingsonderzoek
- Student en leefstijl zorgt met eigen cursussen dat studenten voeding en medicijnen het vak voeding in de zorg kunnen volgen binnen hun opleidingen.
- Suikerconsumptie in voeding is eerder schadelijk dan gunstig voor de gezondheid, vooral bij cardiometabole aandoeningen en kanker heeft toegevoegde suiker schadelijke gevolgen.
- Urinetest kan iemand persoonlijk een voedingspatroon - dieet aanraden. Een zogezegd gepersonaliseerd dieet blijkt uit nieuwe studie.
- Vegetarisch dieet kan klimaat verbeteren en miljoenen mensenlevens redden en kosten gezondheidszorg zouden kunnen dalen met honderden miljarden
- Vegetarische vezelrijke voeding geeft minder risico op diverticulose, afwijkingen aan de darm, blijkt uit grote bevolkingsstudie
- Vetverdeling op het lichaam speelt grotere rol in risico op bepaalde vormen van kanker dan het BMI. Buikvet geeft grootste risico op baarmoederkanker, slokdarmkanker en leverkanker. Heupvet met groter risico op borstkanker.
- Voeding: naleving van verschillende gezonde eetpatronen wordt geassocieerd met een lager risico op totale en oorzaakspecifieke mortaliteit.
- Welke vitamines en mineralen helpen ter voorkoming, preventie van kanker? Een overzicht van belangrijke studies en recente inzichten
- Westerse verschraalde landbouwgrond voorziet de daarop geteelde groenten en fruit niet meer voldoende van noodzakelijke mineralen en vitaminen. Aldus opzienbarend onderzoeksrapport.
- Zwarte bonen bevatten erg veel anti-oxidanten en zijn belangrijk in uw voedingspatroon voor een betere gezondheid.
- Algemeen: Voeding en voedingstoffen die een preventief effect hebben om kanker: te voorkomen. Een aantal studies en aanbevelingen bij elkaar gezet.



Plaats een reactie ...
Reageer op "Foliumzuur via voeding geeft significant minder risico op hormoon-receptor-negatieve borstkanker bij vrouwen in leeftijd voor de overgang"